Burning issues: conclusions and recommendations
This report has focused on THR and the benefits to public and individual health of having available, affordable, appropriate and acceptable safer alternatives to combustible tobacco products. It also focuses on the rights of smokers who need the opportunity to switch from smoking and those who have chosen safer alternatives.
The way forward
For the first time there is now a wider range of positive inducements for people to switch from smoking, rather than just disincentives. THR, through SNP, offers an unprecedented exit strategy that has been shown to be acceptable to smokers and at minimal cost to governments.
Aspirations aside, the reality is that tobacco control could only ever help to reduce harm, so the case for harm reduction has always been inherent in the mission statement for tobacco control: except now there is a real-world opportunity to add enormous heft to beneficial public health outcomes.

Conclusions
- Nearly 8 million people die from smoking-related diseases every year.
- Eighty per cent of the world’s smokers live in LMIC, but have the least access to affordable SNP.
- A projected one billion people will die from smoking-related diseases by 2100.
- Smoking rates have been falling in more affluent countries for decades, but rates of decline are slowing.
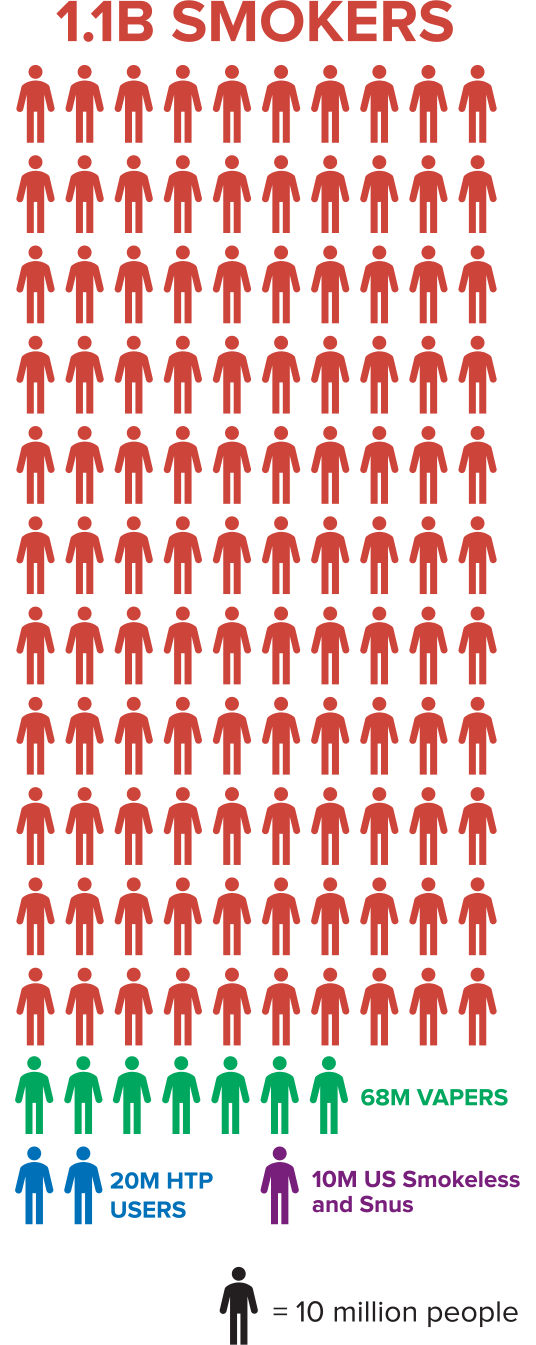
- The global number of smokers has remained unchanged at 1.1 billion since the year 2000, and in some poorer countries this is set to rise due to population growth.
- The immediate way to reduce smoking-related deaths is to focus on current smokers.
- The evidence for SNP demonstrates that they are substantially safer than combustible tobacco, both for smokers and by-standers, and contribute to helping those wishing to stop smoking.
- The adoption of SNP has been consumer-driven with nil, or minimal, cost to governments.
- SNP have the potential to substantially reduce the global toll of death and disease from smoking, and to effect a global public health revolution.
- Progress in the adoption of SNP has been slow. We estimate 98 million people globally use SNP – including 68 million vapers – amounting to only nine per 100 smokers (fewer in LMIC). There is an urgent need to scale up tobacco harm reduction.
- Many well-funded national and international NGOs, public health agencies, and multi-lateral organisations incorrectly view THR as a threat rather than as an opportunity.
- Many US and US-funded organisations have manufactured panics about young people and vaping, about flavours and the outbreak of lung disease, overshadowing the real public health challenge, which is to persuade adult smokers to switch.
- The near-monopoly on international tobacco control funding by US-based foundations – philanthrocapitalism – has distorted international and national responses to smoking. Donor interests often exclude other policy options, producing a hidden but negative impact on health policies, particularly in LMIC.
- The increasingly prohibitionist emphasis risks many consequences, including that current smokers may decide not to switch, current users of SNP may go back to smoking, and the growth of unregulated and potentially unsafe products.
- There continues to be much poorly conducted research and science, which is then spun with an anti-THR message.
- The WHO’s MPOWER initiative alone will be insufficient in hastening an end to smoking – the weakest area of achievement is ‘O’ – offering help – which is also the most expensive for governments.
- Harm reduction is embedded in nearly every field of the WHO’s work except tobacco.
- By denying the role of THR, the WHO is working against the principles and practices enshrined in its own pledges for global health promotion and in international conventions relevant to the right to health, including in Article 1 (d) of the FCTC.
- Richer countries have been the main beneficiaries of THR. Many LMIC are left behind, through a combination of prohibitionist policies and the unavailability of appropriate, acceptable and affordable alternatives to combustible tobacco.
- Those most affected by tobacco control policies have been stigmatised and excluded from the policy conversation. Good public health engages affected populations. The slogan “nothing about us without us” is central to THR, as it is to any field in public health.
Recommendations
- The primary aim of tobacco control should be to offer current smokers suitable exit strategies. The current predicted toll from smoking can only be averted by hastening a switch from smoking by established smokers.
- Harm reduction should be properly defined by parties to the FCTC to sit alongside demand and supply reduction. It should be applied universally with no person, group, or community being excluded.
- The WHO must play a lead role in encouraging FCTC signatories to take a more balanced view of the potential for SNP to help encourage a switch away from combustible products. The current interpretation of Article 5.3 of the FCTC is stifling open debate on the merits of SNP. A new and inclusive approach is required, engaging with all stakeholders with no exceptions, to evaluate the merits of new technologies and products, based on scientific principles rather than ideology
- Access to SNP should be a right for all potential beneficiaries irrespective of gender, race, social or economic circumstances.
- Consumer wellbeing should be at the centre of international planning and policy.
- The Framework Convention Alliance of NGOs should actively engage with the widest range of THR-focused NGOs, including consumer advocacy organisations.
- Companies making SNP should strive to reach the largest number of smokers globally with appropriate and affordable products.
- The role of government should be to hasten the switch from smoking, rather than to place obstacles in the way of those who wish to use SNP.
- No action should be taken which has the consequence of favouring smoking over SNP, such as making SNP harder to obtain and use than cigarettes, or through unfavourable pricing (e.g. through taxes).
- All those in positions to formulate policy on SNP should take account of the body of current evidence, rather than opting for off-the-shelf recommendations from multi-lateral and philanthropic organisations.
- Governments should ensure consumer safety in relation to SNP, based on safety standards available through international, regional and national bodies.
- Smokers have the right to evidence-based information about the potential benefits of switching to SNP.
- SNP should be controlled and regulated as consumer products, and consumers need to be assured of the quality of the products they are using.
- Having a choice of flavours in SNP is an important aspect of the decision to switch away from smoking and to avoid relapse. Banning flavours is counter-productive to positive public health outcomes.
- There is no identified risk of ‘passive vaping’ to bystanders. Public health communication should explain that vaping is not smoking, and ultimately the decision to control vaping in particular locations should be left to individual organisations and businesses, rather than through blanket prohibition by government bodies.
And finally...
The two years since the last edition of this report has been a very difficult time for THR.
The estimated 1.1 billion smokers around the world deserve a better deal and better options. We need to hasten the demise of combustibles and encourage the use of safer non-combustible ways of using nicotine. Evidence from several countries shows that the availability of SNP helps people to switch from smoking.
The two years since the last report has been a very difficult time for tobacco harm reduction.
Globally, progress is slow and those using SNP are still a small fraction of those who smoke. Vaping products have only been on the market for about 12 years and HTP much less, although snus use goes back centuries. Historically, changes in nicotine consumption take some decades. The last disruptive innovation was the invention of the tobacco rolling machine back in the 1880s, but it took around 60 years for the machine-rolled cigarette to oust most other forms of tobacco use in richer countries.
However, we can’t wait 60 years. We know that SNP are just that – safer than getting nicotine by burning tobacco. We know that people want to use these products. We have proof from many countries that THR works.
The obstacles are rich foundations with a myopic view of tobacco control, and international organisations wedded to a narrow view of what can be done. There’s too much fear, hatred and vested interest in this field. These organisations are rapidly finding themselves on the wrong side of history. There needs to be much more ambition about what can be done, along with a healthy dose of compassion.
During the 1980s, public health policies broadened in scope beyond the control of infectious diseases, to wider considerations of prevention through health promotion. In November 1986, the WHO convened the First International Conference on Health Promotion, held in Ottawa, Canada. From that emerged a five-page document called the Ottawa Charter, which defined health promotion,
“as the process of enabling people to increase control over, and to improve, their health”.
It went on to highlight that,
“Health promotion focuses on achieving equity in health. Health promotion action aims at reducing differences in current health status and ensuring equal opportunities and resources…People cannot achieve their fullest health potential unless they are able to take control of those things which determine their health”
THR is good public health and health promotion, starting with the people who matter: smokers and those who have chosen alternatives. It’s change driven from community level upwards – because it’s people who do harm reduction, not experts.
Pledges made by the participants in the Conference included:
- “to counteract the pressures towards harmful products”.
- “to respond to the health gap within and between societies, and to tackle the inequities in health produced by the rules and practices of these societies”.
- “to acknowledge people as the main health resource, to support and enable them to keep themselves, their families and friends healthy”.
Tobacco harm reduction is good public health and health promotion, starting with the people who matter: smokers and those who have chosen alternatives. It’s change driven from community level upwards – because it’s people who do harm reduction, not experts.